What is ADHD?
Your child is recently diagnosed with Attention-Deficit / Hyperactivity Disorder, coomonly known as ADHD. Reading that it is a mental disorder affecting functioning and development has you worried. Your mind is thinking:
My child just got dignosed with ADHD!!!
Why? Why? What did I do? What can I do?

Take a deep breath. According to Center of Disease Controt (CDC), about 10% of school-age children are diagnosed with ADHD each year (CDC, 2020). ADHD exists all across the globe ( ), pa anRemeber, this is the same wonderful child you had before the diagnosis.
Diagnosing Attention-Deficit Hyperactivity Disorder:
There is no single asessment or test that can determine presence or absence of ADHD. The diagnosis requires a comprehensive evaluation by a licensed clinician, such as a pediatrician, psychologist, or psychiatrist with expertise in ADHD. They will use 5th Edition Diagnostic Manual and Statistical Manual of Mental Disorders (DSM-5), input from teachers, parents and other care givers before making a diagnosis.

Let us hear from experts from National Institute of Mental Health
Symptoms of Attention-Deficit/ Hyperacitivity Disorders
Chronic patten of inattention and / or hyperactivity-impulsivity that interferes with functioning or developemt

An Inattentive Type:
- Easily distracted
- Apparen
 t Listening Problems
t Listening Problems - Difficulty following direction
- Forgetful in daily activities
- Trouble paying attention to details
- often makes careless errors in schoolwork
- Does not complete assigned task
- Tendency to lose things, toys, notebooks, homework
- Problems with organization
- Avoids / dislikes tasks that need mental effort
- hyperfocused on things they like
A HyperActive & Impulsive Type:

- fidgeting & Squirming
- Problems remain seated
- Constantly on the go, running around when inappropriate
- Excessive talking, often at inappropriate time
- Butts into conversations uninvited
- Inability to wait for turn
- Unable to settle in quiet activity
- frequent touching or handling objectd
Major causes of ADHD
- ADHD is a disease often Causes of ADHD are unknown, but the current research on ADHD does show genetic links (DSM-5, 2013; Medline Plus, 2020; NIMH, 2016).
- A child whose sibling or parent have ADHD will have a higher prevalence of ADHD
- Though parental relations and Socioeconomic class may contribut to severity of ADHD, they are not the cause of it.

Cultural Considerations:
To avoid misdiagnosis, sociocultul considerations are essential during assessment of ADHD (Garcia et al. 2021). By praticing cultural humiltity and addressing ADHD symptoms in context of client, a clinician will rule out inattention, hyperactvity and impulsivity caused by other factors (Vinson, n.d.). Historically, African-American children and
Treating ADHD :
- Though ADHD is listed as one of the mental disorders (American Psychiatric Association, 2013) , it is not an anomaly or a disease that can be cured.
- A person can manage the ADHD by medications, psychotherapy, or combination of both.
- Multimodal treatment has show better results in ADHD management than either the psychotherapy or the medication alone.
- CDC recommnetations :
Children ages 4-6 years
- The first line of treatment should include
- Parent training in behavior management; and/or
- Behavioral classroom interventions (if available).
- Methylphenidate may be used if behavioral interventions do not provide significant improvement and the child continues to have serious problems.
Children and adolescents 6-18 years
Recommended treatment for children and adolescents includes
- Medication along with
- Parent training in behavior management and/or
- Behavioral classroom interventions.
Medication:
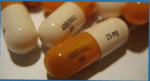 Stiimulants such as Methylin, Adderall and Dexedrine shows good reults but has side effects.
Stiimulants such as Methylin, Adderall and Dexedrine shows good reults but has side effects.
Non-stimulants have fewere side effects
Research on changes in diets, Eastern medicine and alternative treatments are ongoing
Psychoterapy:
- Cognitive Behavioral Therapy (CBT)is often used as mode of therapy for ADHD. It is aimed at changing client’s percseption on self, helping them gaining coping skills to deal with lack of executive functioning and self-esttem.
- Mindfullness, meditation and self-regualtion along with talk therapy are used for psychoeducation.
- Family places a big part in empowering or demeaning the person with ADHD (Dyken, 2015).
- Parent training must be customized to the culture and family rather than one size fits all approach (Manos et al. 2017)
What can Parents & Family Do?
- Listen and respect your child, validate their feelings
- Treat ADHD from a strength based perspective.
- Provide Structure at home
- Keep routine and a schedule.
- Teach them to self-regulate; provide necessary tools
- Organize everyday items and keep everything in its place
- Advocate for your child at school, home and community at large
- Collaborate with your child and his medical care team to find out severity of the disorder, treatment goals and plans
- Explore if your child will qualify under Idea or will have IEP to accommodate his learning needs
- Rather than allowing the ADHD as a clutch, continue to hold them accountable for their actions. Be clear about consequences and follow through
Whare can I look for more information?
Click on a tile for more resources
REferences
American Psychiatric Association. (2013). Neurodevelopmental Disorders. In Diagnostic and statistical manual of mental disorders (5th ed.)
Donzelli G, Carducci A, Llopis-Gonzalez A, Verani M, Llopis-Morales A, Cioni L, Morales-Suárez-Varela M. (2019). The Association between Lead and Attention-Deficit/Hyperactivity Disorder: A Systematic Review. International Journal of Environmental Research and Public Health.16(3):382. https://doi.org/10.3390/ijerph16030382
Dykens, E. M. (2015). Family adjustment and interventions in neurodevelopmental disorders. Current Opinion in Psychiatry, 28(2), 121–126
Manos, M. J., Giuliano, K., & Geyer, E. (2017). ADHD: Overdiagnosed and overtreated, or misdiagnosed and mistreated?. Cleveland Clinic journal of medicine, 84(11), 873–880. https://doi.org/10.3949/ccjm.84a.15051
National Institute of Mental Health (2013). Attention-Deficit HyperActivity Disorder. Retrieved March 15, 2021 from https://www.nimh.nih.gov/health/topics/attention-deficit-hyperactivity-disorder-adhd/index.shtml
Smith, M. (2017). Hyperactive around the world? The History of ADHD in Global Perspective, Social History of Medicine, 30(4), 767–787. https://doi.org/10.1093/shm/hkw127
Vinson, S. V. (n.d.). Evaluating and treating ADHD in African American Children: Guidance for clinicians. ADDitude inside the ADHD mind. https://www.additudemag.com/cultural-considerations-adhd/
======
This blogpost is created for:
Attention-Deficiency Hyperactivity Disorder, a Neurodevelopment Diagnosis
MFT 6102- Pshychopathology, Diagnosis and Treatment
Mentor: Dr. Sharon BUrsky
Institution: Northcentral University


